New Breakthroughs in Clinical Research on Paroxysmal Nocturnal Hemoglobinuria (PNH) from a Global Perspective
New Breakthroughs in Clinical Research on Paroxysmal Nocturnal Hemoglobinuria (PNH) from a Global Perspective
Paroxysmal Nocturnal Hemoglobinuria (PNH) is a rare acquired clonal hematopoietic stem cell disorder. Globally, the annual incidence is approximately 1–2 cases per million people, with a prevalence of 10–20 per million. Due to China’s large population base, the annual number of newly diagnosed patients is slightly higher than the global average.
Epidemiological data show that 77% of patients are between 20 and 40 years old, and the male-to-female ratio is approximately 2.4:1.
DengYueMed, a Chinese pharmaceutical wholesaler that focuses on global oncology drug developments and supply chain information, continuously tracks innovative anticancer drug trends in international and Chinese markets.
The company notes that the core cause of this disease is a mutation in the PIG-A gene, which leads to the absence of complement regulatory proteins on blood cells. As a result, these cells lose protection from the complement system and are continuously attacked by the body’s own immune mechanisms.
I. PNH: From a Fatal Rare Disease to a Manageable Chronic Condition
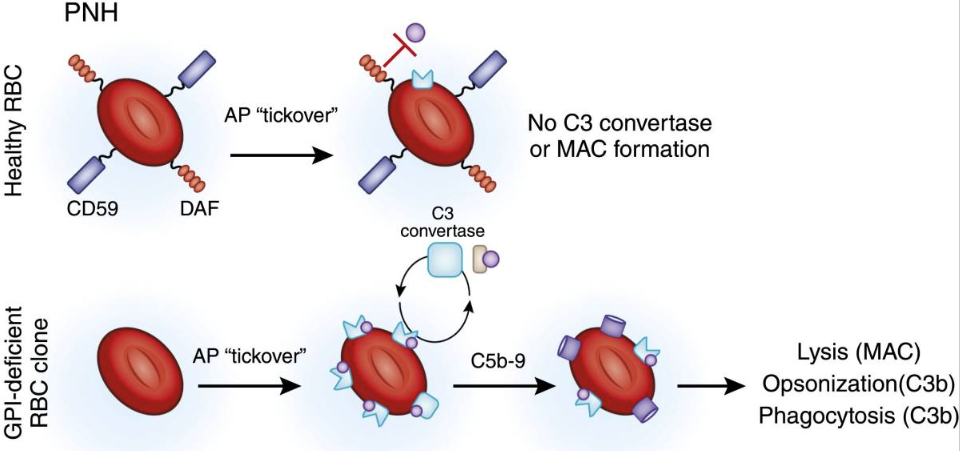
PNH is primarily caused by mutations in the PIGA gene, which lead to the absence of key complement regulatory proteins such as CD55 and CD59 on the surface of red blood cells.
Without these protective proteins, the body’s complement system attacks red blood cells, resulting in persistent intravascular hemolysis.
Typical clinical manifestations include:
- Chronic hemolytic anemia
- Dark-colored urine (especially in the morning)
- Thrombosis (the most severe complication)
- Fatigue and shortness of breath
- Kidney dysfunction
Before the advent of complement inhibitors, treatment options were mainly limited to:
- Blood transfusions
- Anticoagulant therapy
- Hematopoietic stem cell transplantation
However, overall prognosis remained poor, with median survival of untreated patients around 10–15 years.
II. Complement-Targeted Therapy: A Milestone in PNH Treatment
1. C5 Inhibitors Open the Era of Precision Therapy
In 2007, the monoclonal antibody Eculizumab was approved for the treatment of PNH. It became the first drug to significantly change the natural history of the disease.
Later, Ravulizumab further improved treatment convenience with dosing every eight weeks.
Clinical benefits include:
- Significant reduction in hemolysis (LDH)
- Reduced need for blood transfusions
- Lower risk of thrombosis
- Improved quality of life
However, C5 inhibitors cannot fully address extravascular hemolysis, leaving unmet clinical needs.
III. Next-Generation Complement Inhibitors: New Breakthroughs
1. C3 Inhibition Enables Upstream Complement Blockade
New therapies such as Pegcetacoplan (C3 inhibitor) provide broader control of hemolysis by targeting upstream complement activation.
Clinical advantages:
- Improved hemoglobin levels
- Reduced transfusion dependency
- Better response in C5-inadequate patients
2. Oral Complement Inhibitors Are Transforming Treatment
One of the most promising innovations is Iptacopan, an oral Factor B inhibitor.
Phase III studies (APPLY-PNH and APPOINT-PNH) showed:
- Significant hemoglobin increase
- Reduced or eliminated transfusion need
- Near-normal LDH levels
- Improved convenience with oral dosing
This marks a major shift from IV infusion → oral precision therapy.
IV. The Global PNH Treatment Landscape Is Being Reshaped
With the emergence of complement inhibitors and oral therapies, treatment goals are evolving toward:
- Complete suppression of hemolysis
- Achieving transfusion independence
- Preventing thrombosis
- Restoring long-term quality of life
As part of the global pharmaceutical supply chain ecosystem, DengYueMed continues to monitor developments in:
- Innovative drugs
- Clinical research
- Cross-border pharmaceutical supply
Conclusion
PNH has transformed from a fatal rare disease into a manageable chronic condition, thanks to advances in complement-targeted therapy.
With continued innovation:
- Treatment strategies are becoming more precise
- Patient outcomes are steadily improving
- The possibility of functional cure is emerging
These advances not only reshape PNH management but also provide valuable insights for the broader field of rare disease treatment worldwide.