Targeting TL1A in Immune-Mediated Inflammatory Diseases: From an Inflammatory Amplifier to a New Strategy for Precision Intervention
In the field of immune-mediated inflammatory diseases (IMIDs), such as inflammatory bowel disease (IBD), rheumatoid arthritis, and psoriasis, biologics targeting TNF, IL-6, and IL-17 have significantly improved patient outcomes. However, a considerable proportion of patients still experience inadequate responses or develop resistance. Therefore, identifying upstream regulatory targets with broader immunomodulatory capacity has become a key focus in modern immunotherapy. In this context, TL1A (TNF-like ligand 1A), as a critical immune regulator, is emerging as a next-generation therapeutic target.
Ⅰ. What is TL1A?
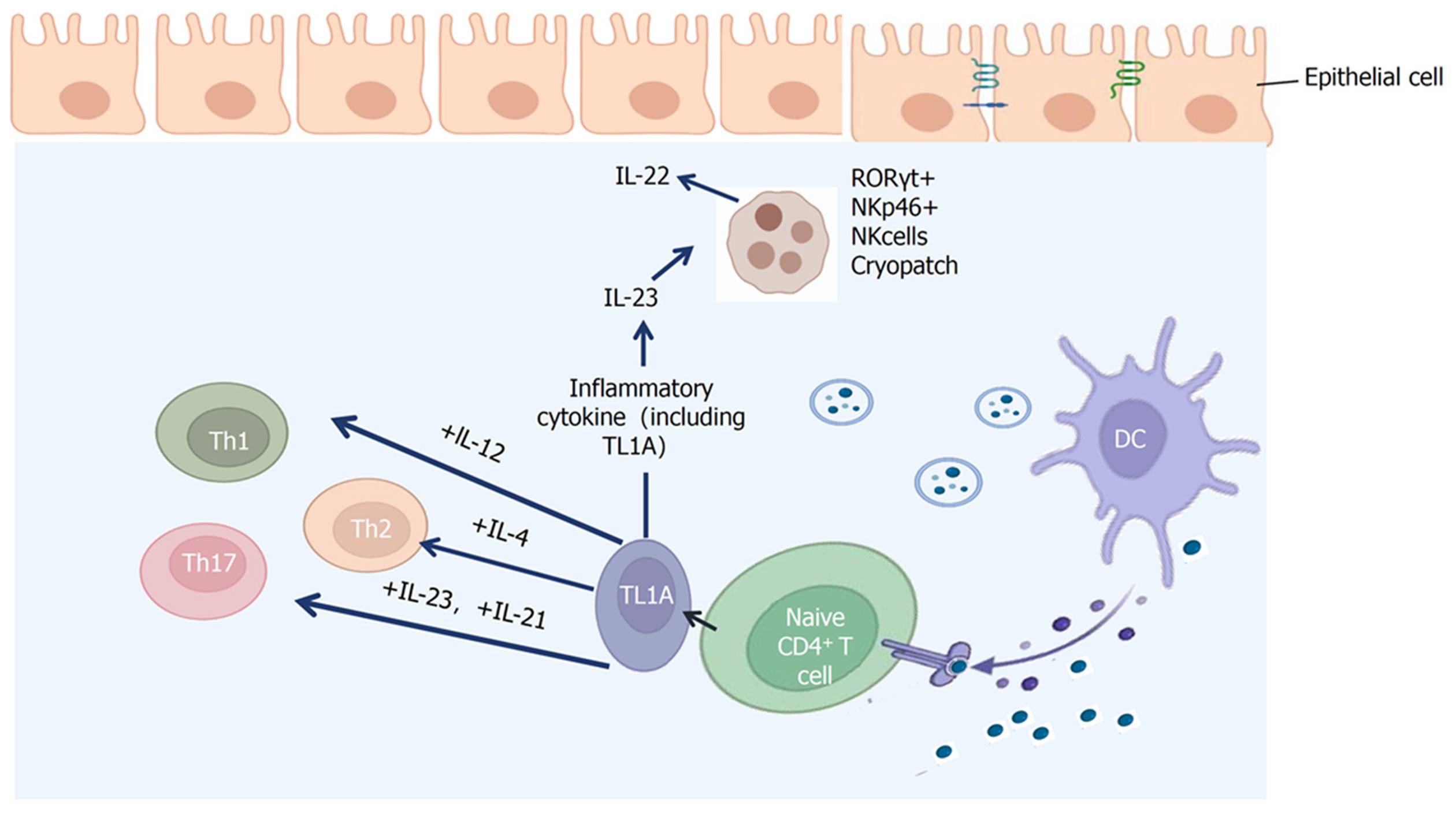
TL1A (also known as TNFSF15) is a member of the tumor necrosis factor (TNF) superfamily. It is primarily produced by antigen-presenting cells (such as dendritic cells and macrophages) as well as endothelial cells. Its main receptor is DR3 (Death Receptor 3), and their interaction activates multiple immune signaling pathways.
The TL1A–DR3 axis plays several roles in the immune system:
● Promotes T cell activation and proliferation
● Enhances Th1 and Th17 inflammatory responses
● Regulates innate lymphoid cell (ILC) function
● Participates in intestinal mucosal immunity
● Amplifies inflammatory cascades
Under normal conditions, TL1A contributes to immune defense and tissue repair. However, in chronic inflammatory diseases, its overexpression leads to dysregulated immune responses, making it a key driver of persistent inflammation.
Ⅱ. Why is TL1A a Key Therapeutic Target?
1. A potent “amplifier” of inflammation
TL1A acts upstream in inflammatory signaling and can simultaneously enhance multiple immune pathways (e.g., Th1, Th17, ILC2). This means it not only initiates inflammation but also amplifies ongoing immune responses.
2. Strong association with multiple diseases
● Elevated TL1A levels have been observed in various IMIDs, including:
Inflammatory bowel disease (Crohn’s disease and ulcerative colitis)
● Rheumatoid arthritis
● Psoriasis
● Asthma and allergic diseases
In IBD particularly, TL1A is closely associated with intestinal fibrosis, persistent inflammation, and disease severity.
3. Genetic evidence supports its role
Polymorphisms in the TNFSF15 gene are strongly linked to IBD susceptibility, providing solid genetic support for TL1A as a therapeutic target.
👉 Therefore, TL1A is not only a participant in inflammation, but also a disease driver.
Ⅲ. Mechanism of Action of TL1A-Targeted Therapies
Therapies targeting TL1A (such as anti-TL1A monoclonal antibodies) primarily work by blocking the interaction between TL1A and DR3, thereby suppressing downstream inflammatory signaling.
Key mechanisms include:
1️⃣ Inhibition of T cell overactivation
Blocking TL1A reduces Th1 and Th17 activity, lowering the release of inflammatory cytokines such as IFN-γ and IL-17.
2️⃣ Suppression of inflammatory cascades
By inhibiting an upstream “amplifier,” multiple inflammatory pathways are downregulated simultaneously, leading to systemic anti-inflammatory effects.
3️⃣ Improvement of tissue damage and fibrosis
In IBD, TL1A is closely linked to intestinal fibrosis. Its inhibition may help restore normal tissue structure.
4️⃣ Restoration of immune balance
Some studies suggest that TL1A blockade may enhance regulatory T cell (Treg) function, helping re-establish immune tolerance.
👉 Fundamentally, TL1A-targeted therapy represents not just “inflammation suppression,” but “immune network remodeling.”
Ⅳ. Clinical Development Progress
Several anti-TL1A monoclonal antibodies are currently in clinical development, particularly for IBD.
1. Inflammatory Bowel Disease (IBD)
● Clinical studies have shown: Significant improvement in clinical remission rates
● Enhanced endoscopic mucosal healing
● Efficacy in patients who failed anti-TNF therapies
● Potential benefits in fibrosis-related outcomes
2. Safety profile
● Preliminary data indicate: Generally manageable adverse events
● Lower infection risk compared to some broad immunosuppressants
● No clear signs of excessive immune suppression
👉 These findings suggest strong clinical potential for TL1A-targeted therapies.
Ⅴ. Differences from Existing Biologics
| Dimension | Anti-TNF / Anti-IL-6 Therapies | TL1A-Targeted Therapy |
|---|---|---|
| Target level | Downstream cytokines | Upstream regulator |
| Scope of action | Limited pathways | Multi-pathway modulation |
| Effect on fibrosis | Limited | Potential improvement |
| Patient coverage | Partial response | Potentially broader |
| Mechanistic depth | Inflammation suppression | Immune network remodeling |
👉 TL1A represents a shift from “blocking inflammation” to “controlling the immune system.”
Ⅵ. Potential Expanded Indications
Beyond IBD, TL1A-targeted therapies may expand into:
● Rheumatoid arthritis
● Psoriasis and psoriatic arthritis
● Systemic lupus erythematosus
● Asthma and allergic diseases
● Fibrosis-related disorders
Its value lies in being a broad-spectrum immune regulatory target with platform potential.
Ⅶ. Challenges Ahead
Despite its promise, several challenges remain:
-
Patient stratification
● Not all patients are TL1A-dependent
● Biomarkers are needed -
Long-term safety
● Requires further validation -
Combination strategies
● Needs optimization with other therapies
Ⅷ. Future Directions
Future development of TL1A-targeted therapies will focus on:
✔ Precision medicine approaches
✔ Combination therapies
✔ Early intervention
✔ Anti-fibrotic applications
Conclusion
Targeting TL1A represents a paradigm shift in the treatment of immune-mediated inflammatory diseases—from blocking individual cytokines to regulating upstream immune networks. The promising clinical signals observed in diseases like IBD suggest that TL1A could become a cornerstone of next-generation therapies.
As research advances and clinical data accumulate, TL1A-targeted therapies are expected to provide new options for patients with difficult-to-treat conditions. In the context of accelerating global pharmaceutical innovation, platforms like DengYueMed are helping bridge access to cutting-edge treatments by integrating international resources and compliant service systems, ultimately supporting broader adoption of precision medicine.