Latest Clinical Trial Update and Real-World Cases: Which CAR-T, Bispecific Antibody, and Gene Therapies Are Accessible to Patients?
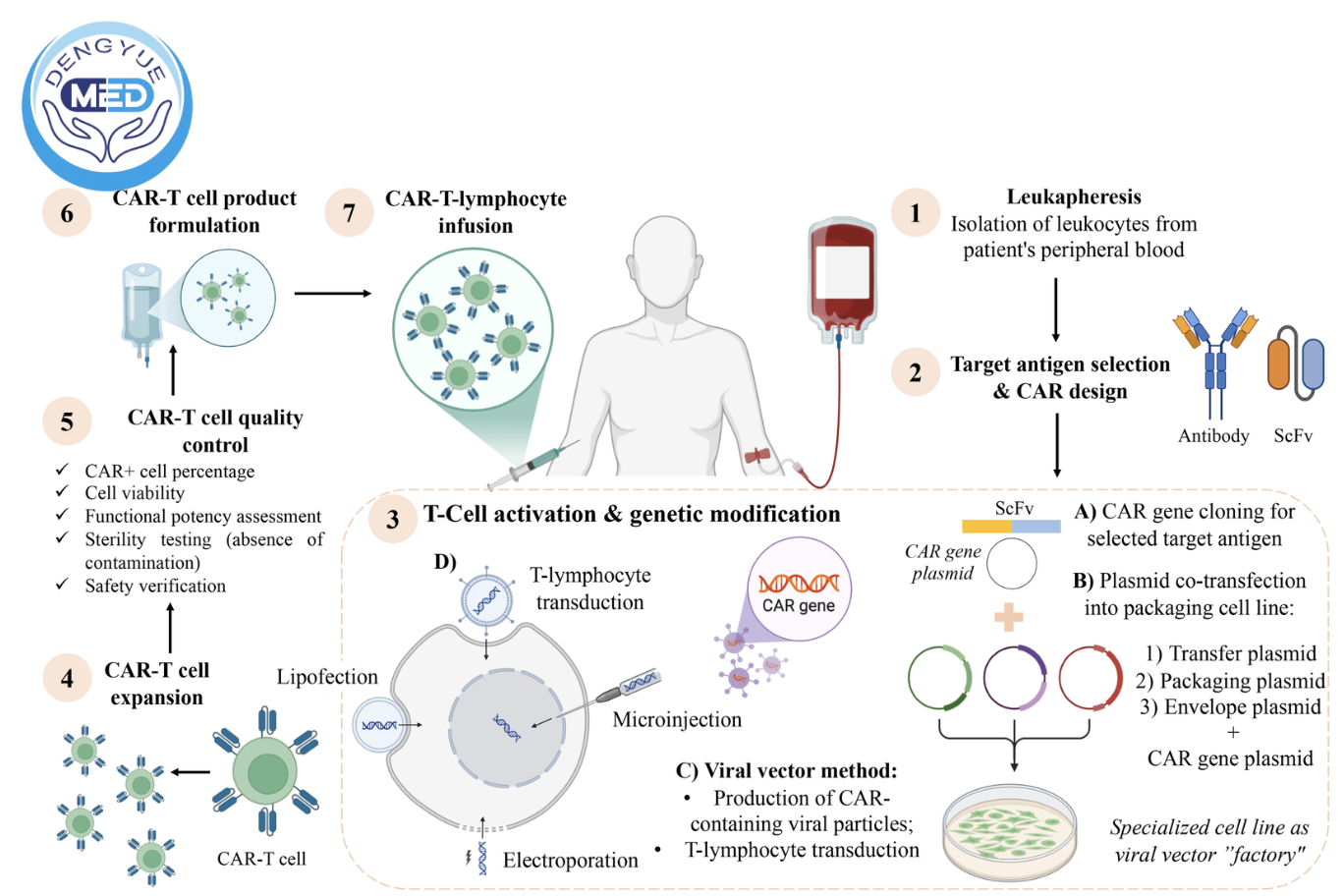
Latest Clinical Trial Update and Real-World Cases: Which CAR-T, Bispecific Antibody, and Gene Therapies Are Accessible to Patients?
| **Frontier Therapy Weekly | Week 1, April 2026 (Issue 6)** |
As of April 2026, clinical development across CAR-T cell therapy, bispecific antibodies (BsAbs), and gene editing technologies continues to accelerate globally.
China has emerged as one of the most active regions in cell and gene therapy research, with over 115 ongoing or recruiting clinical trials. These studies primarily focus on:
●Relapsed/refractory hematologic malignancies
●Advanced solid tumors
●Rare diseases and autoimmune disorders
Beyond technological innovation—such as in vivo CAR-T, dual-target designs, and low-dose strategies—a key shift is underway:
improving real-world patient access to early-stage advanced therapies.
This article reviews key recruiting trials in April 2026, alongside selected real-world clinical observations, to help assess which patient populations may benefit and under what conditions.
1. CAR-T Therapy: Expanding Access Through Dual Targeting, In Vivo Engineering, and Dose Optimization
Clinical Recruitment Trends
The current evolution of CAR-T is no longer limited to efficacy validation, but increasingly focused on broadening eligible patient populations and improving safety profiles.
1) Solid tumor CAR-T programs advancing
●Ongoing trials are recruiting patients with:
Gastric and gastroesophageal cancers (CLDN18.2)
●Hepatocellular carcinoma (GPC3)
●Pancreatic cancer (multi-target immune modulation)
Early real-world and clinical data suggest that CLDN18.2-targeted CAR-T therapies may achieve clinically meaningful response and disease control rates in selected patients.
2) In vivo CAR-T entering early clinical stages
Emerging programs (e.g., TGI-5 and similar platforms) are evaluating direct in vivo generation of CAR-T cells, characterized by:
●Elimination of ex vivo cell processing
●Single-dose intravenous administration
●Significantly reduced manufacturing timelines
These approaches may be particularly relevant for patients with rapid disease progression who cannot wait for conventional production timelines.
3) Low-dose and allogeneic CAR-T strategies
●Dose-reduction strategies (e.g., ~5×10⁶/kg) are being evaluated to mitigate CRS and ICANS risks
●Allogeneic (“off-the-shelf”) CAR-T products are under investigation to improve scalability and availability
4) Expansion into autoimmune diseases
CAR-T trials are increasingly including patients with:
●Systemic lupus erythematosus (SLE)
●Membranous nephropathy
This reflects a broader shift toward immune system reprogramming beyond oncology.
Real-World Clinical Observations
●A 70-year-old patient with relapsed/refractory multiple myeloma treated with dual-target BCMA/CD19 CAR-T achieved complete response (CR) within 72 hours, with sustained remission beyond 6 months and only mild fever reported.
●A patient with advanced gastric cancer enrolled in a CLDN18.2 CAR-T trial demonstrated tumor shrinkage and improved quality of life, with progression-free survival exceeding 4 months at the time of reporting.
Potentially Eligible Patients
●Relapsed/refractory hematologic malignancies (e.g., lymphoma, multiple myeloma)
●Advanced solid tumors (e.g., gastric, liver, pancreatic cancers)
●Selected autoimmune disease populations
Eligibility typically requires biomarker or target expression confirmation (e.g., BCMA, CLDN18.2).
2. Bispecific Antibodies: From Alternative Option to Core Therapeutic Strategy
Compared to CAR-T, bispecific antibodies offer immediate availability and standardized administration, making them increasingly central in treatment pathways.
Clinical Recruitment Trends
1) PD-1/VEGF bispecifics expanding indications
Programs such as ivonescimab are being evaluated in:
●Brain metastases
●Multiple solid tumor subtypes
New recruitment sites continue to open in April.
2) Growth in multi-target bispecifics
Clinical trials are ongoing across:
●Gastric cancer
●Colorectal cancer
●Non-small cell lung cancer
China remains a global leader in the number of bispecific antibody trials, particularly in colorectal cancer.
3) Combination strategies gaining momentum
Bispecific antibodies are increasingly used in combination settings:
●As bridging or sequential therapy before CAR-T
●In combination with antibody-drug conjugates (ADCs)
●Alongside immune checkpoint inhibitors
Real-World Clinical Observations
●A patient with advanced colorectal cancer treated with PD-1-based bispecific therapy achieved partial response (PR), with progression-free survival exceeding 12 months and manageable toxicity.
●A gastric cancer patient received bispecific antibody therapy for disease control prior to CAR-T treatment and subsequently achieved complete remission.
Potentially Eligible Patients
●Advanced solid tumor patients (gastric, colorectal, lung cancers)
●HER2-positive or PD-L1–expressing populations
●Patients intolerant to or refractory to chemotherapy
In clinical practice, bispecific antibodies often function as a bridging or complementary therapy.
3. Gene Therapy: Expanding from Rare Diseases to Oncology Applications
Gene editing technologies, particularly CRISPR/Cas-based approaches, are steadily progressing toward clinical application.
Clinical Recruitment Trends
1) In vivo gene editing trials initiated
Programs targeting conditions such as MYOC mutation-related glaucoma (e.g., BD113) and selected oncology indications have entered early clinical phases.
2) Continued progress in rare disease therapies
Includes:
●Beta-thalassemia
●Duchenne muscular dystrophy
Some approaches are exploring one-time curative treatment models.
3) Integration with CAR-T therapy
Gene editing is being used to:
●Enhance CAR-T persistence
●Reduce immunogenicity
●Improve safety profiles
Real-World Clinical Observations
●A pediatric patient with a genetic eye disorder treated with CRISPR-based therapy showed stabilized intraocular pressure and improved visual function, with no severe adverse events reported.
●An adult oncology patient receiving gene-editing–enhanced therapy achieved durable disease control when combined with immunotherapy.
Potentially Eligible Patients
●Patients with defined pathogenic genetic mutations (rare diseases)
●Advanced cancer patients with actionable molecular profiles
●Candidates for enhanced cellular therapies
4. Key Barriers to Clinical Trial Access
Despite the increasing number of trials, access remains limited by several factors:
●Strict inclusion and exclusion criteria
●Requirement for biomarker or genetic matching
●Limited enrollment windows
●Operational and logistical complexity
In practice, trial availability does not automatically translate into patient access.
5. From Trial Availability to Enrollment: The Role of Structured Matching
A critical gap remains between clinical trial awareness and successful enrollment.
This gap often involves:
●Identifying appropriate trials based on disease profile
●Interpreting eligibility criteria
●Preparing medical documentation
●Coordinating with trial centers
Dengyuemed focuses on bridging this gap through:
●Systematic tracking of global CAR-T, bispecific antibody, and gene therapy trials
●Patient-specific trial matching based on clinical and molecular data
●Preliminary eligibility assessment and documentation support
●Coordination with clinical research centers
Such structured approaches can improve the efficiency of identifying and accessing appropriate investigational therapies.
6. Conclusion
The current wave of innovation across CAR-T, bispecific antibodies, and gene therapy is reshaping the therapeutic landscape.
These advanced treatments are gradually transitioning from limited experimental options to structured, evaluable clinical pathways.
For patients, timely access to accurate information and professional assessment remains essential for navigating increasingly complex treatment options.
Disclaimer
This article is based on publicly available clinical trial data (e.g., ClinicalTrials.gov and related registries) and published findings as of March 2026. Trial availability, eligibility criteria, and treatment protocols are subject to change. All therapeutic decisions should be made in consultation with qualified healthcare professionals.